Why aren’t there varicose arteries – Varicose veins, characterized by swollen and twisted veins, are a common affliction affecting millions worldwide. However, it is intriguing to note that arteries, the blood vessels responsible for carrying oxygenated blood away from the heart, do not exhibit this condition.
This raises the fundamental question: why aren’t there varicose arteries? Delving into the intricate mechanisms of the circulatory system, this article aims to provide a comprehensive understanding of the factors contributing to this phenomenon.
Arteries and veins, despite their complementary roles in blood circulation, possess distinct structural and functional properties. Understanding these differences is crucial in unraveling the mystery behind the absence of varicose arteries.
Absence of Pressure in Arteries
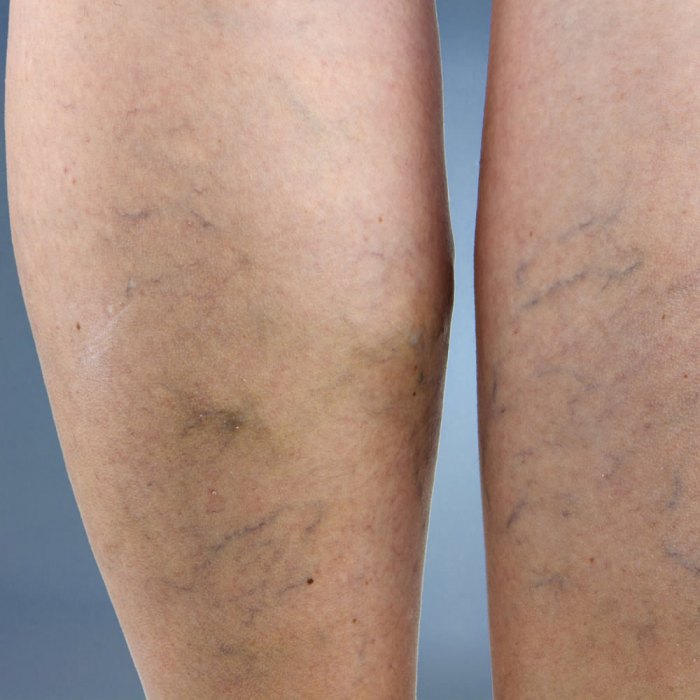
Arteries, unlike veins, do not experience the same pressure fluctuations that lead to varicose veins. This is due to several factors related to the inherent differences in pressure between arteries and veins, as well as the mechanisms that regulate blood flow and pressure in the arterial system.
Pressure Differences between Arteries and Veins
Arteries are responsible for carrying oxygenated blood away from the heart to the body’s tissues and organs. The pressure within arteries is significantly higher than in veins, as the heart pumps blood into the arteries with great force. This high pressure is necessary to overcome the resistance of the blood vessels and ensure adequate blood flow to all parts of the body.
Veins, on the other hand, carry deoxygenated blood back to the heart. The pressure within veins is much lower than in arteries, as the blood flows passively towards the heart due to gravity and the action of muscle contractions. This lower pressure is sufficient for venous return, as the blood does not need to overcome significant resistance.
Mechanisms Regulating Blood Flow and Pressure in Arteries
The arterial system is equipped with several mechanisms that regulate blood flow and pressure, ensuring that tissues and organs receive an adequate supply of oxygenated blood. These mechanisms include:
- Heart rate and stroke volume:The heart rate and stroke volume (the amount of blood pumped out with each beat) determine the overall cardiac output, which is the volume of blood pumped per minute. An increase in cardiac output leads to increased arterial pressure.
- Arterial resistance:The resistance of the arteries to blood flow is regulated by the smooth muscle cells in their walls. When these muscles contract, the arteries narrow, increasing resistance and raising blood pressure. Conversely, when the muscles relax, the arteries widen, reducing resistance and lowering blood pressure.
- Neurohumoral regulation:The nervous system and hormones play a role in regulating arterial pressure. The sympathetic nervous system releases hormones that cause arterial constriction, while the parasympathetic nervous system releases hormones that cause arterial dilation.
Role of Valves in Veins and Absence in Arteries
Veins contain one-way valves that prevent blood from flowing backward. These valves are absent in arteries. The presence of valves in veins is crucial for preventing the accumulation of blood and the formation of varicose veins. In arteries, the absence of valves and the high pressure within the vessels prevent the formation of varicose arteries.
Arterial Wall Structure
The structure of arterial walls differs significantly from that of vein walls, contributing to their resistance to varicosities.
Composition of Arterial Walls
Arterial walls are composed of three layers:
- Tunica intima:The innermost layer, lined with endothelial cells, which are in direct contact with the blood.
- Tunica media:The middle layer, composed primarily of smooth muscle cells that control the diameter of the artery.
- Tunica adventitia:The outermost layer, composed of connective tissue, which provides structural support and protection.
Role of Collagen, Elastin, and Smooth Muscle
Arterial walls contain a high concentration of collagen and elastin, which provide strength and elasticity. Collagen fibers provide tensile strength, while elastin fibers allow the arteries to stretch and recoil. The smooth muscle cells in the tunica media can contract and relax, adjusting the diameter of the artery and regulating blood flow.
Impact of Age and Lifestyle Factors
With age, the composition and structure of arterial walls change. Collagen fibers become stiffer, and elastin fibers lose their elasticity. This can lead to a decrease in arterial compliance, which is the ability of the arteries to expand and contract.
Lifestyle factors, such as smoking and high blood pressure, can also damage arterial walls and increase the risk of varicose vein development.
Blood Flow Dynamics
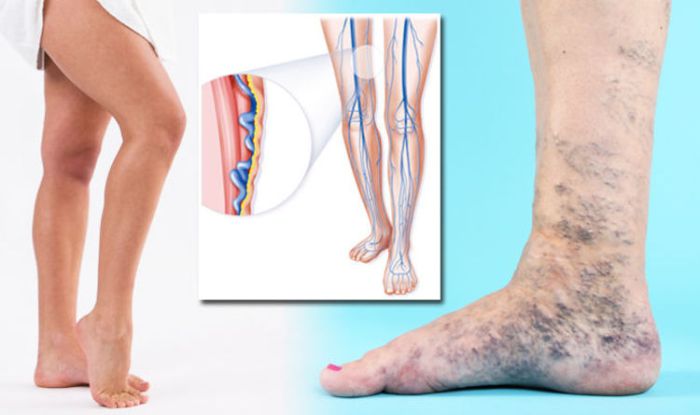
The flow of blood in arteries differs from that in veins, contributing to the resistance of arteries to varicosities.
Laminar Flow in Arteries
Blood flow in arteries is laminar, meaning it flows in layers with no turbulence. This is due to the high pressure and the smooth inner lining of the arteries. Laminar flow reduces friction and minimizes the formation of clots, which can lead to varicose veins.
Factors Influencing Blood Viscosity, Why aren’t there varicose arteries
Blood viscosity, the thickness of the blood, can influence arterial health. High blood viscosity increases resistance to flow and can lead to the formation of varicose veins. Factors that can increase blood viscosity include dehydration, high levels of cholesterol, and certain medical conditions.
Venous-Arterial Communication: Why Aren’t There Varicose Arteries
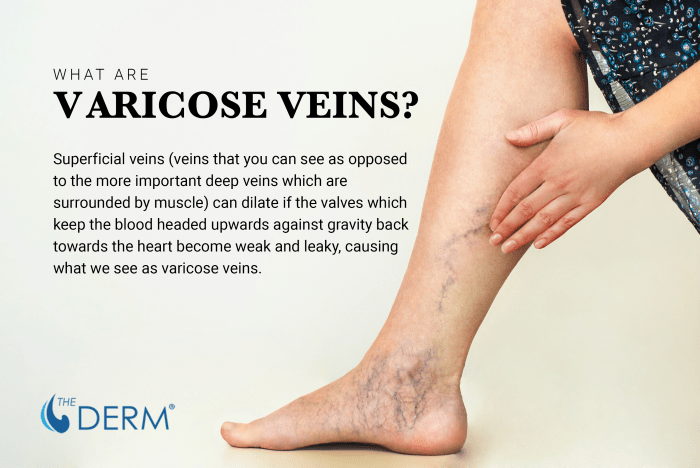
Venous-arterial communication refers to the connections between veins and arteries. These connections can influence the development of varicose veins.
Anatomical Connections
Venous-arterial communication occurs through arteriovenous anastomoses (AVAs), which are small vessels that connect arteries and veins. AVAs play a role in regulating blood flow and temperature.
Role of AVAs in Venous Return
AVAs contribute to venous return by allowing blood to bypass the capillary network and flow directly from arteries to veins. This can reduce the pressure in the veins and help prevent varicose vein formation.
Abnormal Venous-Arterial Communication
Abnormal venous-arterial communication, such as the presence of large AVAs, can lead to varicose vein formation. These abnormal connections can allow high-pressure arterial blood to flow into the veins, increasing venous pressure and damaging the vein walls.
Hormonal Influences
Hormones can play a role in the development of varicose veins.
Effects of Estrogen and Progesterone
Estrogen and progesterone, hormones produced by the ovaries, can affect vein health. Estrogen can weaken the vein walls, while progesterone can increase blood viscosity. These hormonal changes can contribute to varicose vein formation, particularly during pregnancy and menopause.
Hormonal Changes during Pregnancy and Menopause
During pregnancy, the levels of estrogen and progesterone increase significantly. This can lead to a weakening of the vein walls and an increased risk of varicose vein formation. During menopause, the decline in estrogen levels can also contribute to varicose vein development.
Lifestyle and Environmental Factors
Lifestyle and environmental factors can contribute to the development of varicose veins.
Impact of Obesity, Smoking, and Physical Inactivity
Obesity, smoking, and physical inactivity can all increase the risk of varicose vein formation. Obesity puts pressure on the veins in the legs, while smoking damages the vein walls. Physical inactivity can lead to poor circulation and increased venous pressure.
Role of Environmental Factors
Environmental factors, such as prolonged standing or sitting, can also contribute to varicose vein formation. Prolonged standing can increase the pressure in the veins of the legs, while prolonged sitting can lead to poor circulation.
FAQ Insights
Why do varicose veins occur in veins but not in arteries?
Varicose veins occur due to weakened vein walls and malfunctioning valves, which allow blood to pool and cause the veins to enlarge. Arteries, on the other hand, have thicker and more elastic walls, and their valves are more effective in preventing blood from flowing backward, reducing the risk of varicosities.
What factors contribute to the absence of varicose arteries?
The absence of varicose arteries is attributed to several factors, including higher pressure in arteries compared to veins, the structural composition of arterial walls, laminar blood flow, and the absence of hormonal influences that affect vein health.
Can lifestyle factors influence the development of varicose veins?
Certain lifestyle factors, such as obesity, smoking, and prolonged standing or sitting, can contribute to the development of varicose veins by increasing pressure on the veins and weakening their walls.